Welcome to the Resource Center featuring:
Blogs
Read our thought-provoking articles and insights.
(Utilize the filters below to navigate through our entire collection of resources.)
No results found.
We searched high and low, but didn’t find matches to your request.
Please adjust your search criteria to see other results.

04/29/21
Read
07/01/21
Read
09/20/21
Read
10/07/21
Read
12/17/21
Read
01/20/22
Read
02/08/22
Read
02/08/22
Read
03/14/22
Read
03/28/22
Read
03/29/22
Read
03/29/22
Read
03/29/22
Read
03/30/22
Read
03/30/22
Read
04/07/22
Read
04/25/22
Read
05/10/22
Read
05/11/22
Read
05/11/22
Read
05/11/22
Read
05/11/22
Read
05/13/22
Read
06/20/22
Read
06/26/22
Read
06/26/22
Read
06/26/22
Read
06/26/22
Read
06/27/22
Read
06/28/22
Read
06/28/22
Read
06/28/22
Read
06/29/22
Read
06/29/22
Read
07/06/22
Read
07/11/22
Read
08/11/22
Read
08/11/22
Read
08/11/22
Read
08/11/22
Read
08/11/22
Read
08/11/22
Read
08/12/22
Read
08/22/22
Read
09/01/22
Watch
09/03/22
Watch
09/07/22
Read
09/09/22
Watch
09/13/22
Read
09/14/22
Read
09/29/22
Watch
10/01/22
Watch
10/01/22
Read
10/03/22
Read
10/06/22
Read
10/10/22
Read
10/11/22
Read
10/13/22
Read
10/18/22
Read
10/19/22
Watch
11/01/22
Read
11/02/22
Watch
11/02/22
Read
11/07/22
Read
11/09/22
Read
11/12/22
Read
11/15/22
Read
11/16/22
Watch
11/17/22
Watch
11/30/22
Read
11/30/22
Watch
12/02/22
Read
12/05/22
Read
12/06/22
Read
12/13/22
Read
12/14/22
Watch
12/20/22
Read
12/22/22
Read
01/01/23
Watch
01/01/23
Watch
01/03/23
Watch
01/04/23
Watch
01/11/23
Watch
01/12/23
Read
01/13/23
Read
01/23/23
Read
01/24/23
Read
01/25/23
Watch
01/30/23
Read
02/08/23
Read
02/08/23
Watch
02/10/23
Read
02/14/23
Read
02/15/23
Read
02/15/23
Watch
02/15/23
Read
02/20/23
Watch
02/20/23
Read
02/22/23
Watch
02/27/23
Read
03/01/23
Read
03/01/23
Read
03/08/23
Watch
03/13/23
Read
03/14/23
Read
03/15/23
Read
03/15/23
Read
03/21/23
Read
03/22/23
Watch
03/29/23
Read
04/10/23
Read
04/11/23
Read
04/11/23
Read
04/12/23
Watch
04/17/23
Read
04/18/23
Read
04/18/23
Read
04/19/23
Watch
04/24/23
Read
04/24/23
Read
04/24/23
Read
04/27/23
Read
05/03/23
Read
05/03/23
Read
05/05/23
Read
05/11/23
Watch
05/17/23
Read
05/24/23
Watch
05/25/23
Read
05/25/23
Read
06/01/23
Watch
06/01/23
Watch
06/01/23
Watch
06/01/23
Watch
06/06/23
Read
06/07/23
Read
06/12/23
Read
06/12/23
Watch
06/14/23
Read
06/21/23
Watch
06/21/23
Watch
06/23/23
Read
06/23/23
Watch
06/23/23
Read
06/27/23
Read
07/01/23
Read
07/06/23
Watch
07/06/23
Read
07/11/23
Read
07/12/23
Watch
07/13/23
Read
07/21/23
Read
07/23/23
Read
07/24/23
Read
07/25/23
Watch
08/08/23
Read
08/09/23
Read
08/09/23
Watch
08/11/23
Read
08/14/23
Read
08/15/23
Read
08/15/23
Read
08/22/23
Read
08/23/23
Watch
08/23/23
Read
08/23/23
Read
08/30/23
Read
08/30/23
Read
09/01/23
Watch
09/08/23
Read
09/11/23
Read
09/13/23
Watch
09/13/23
Read
09/13/23
Watch
09/20/23
Read
09/20/23
Watch
09/23/23
Read
09/27/23
Watch
09/29/23
Watch
10/02/23
Watch
10/03/23
Watch
10/06/23
Read
10/09/23
Watch
10/10/23
Read
10/11/23
Watch
10/13/23
Watch
10/18/23
Read
10/18/23
Watch
10/20/23
Watch
10/21/23
Read
10/23/23
Read
10/24/23
Watch
10/25/23
Watch
10/27/23
Watch
10/30/23
Read
10/31/23
Read
11/01/23
Learn More
11/01/23
Watch
11/01/23
Watch
11/01/23
Watch
11/01/23
Read
11/01/23
Read
11/01/23
Read
11/01/23
Watch
11/02/23
Learn More
11/02/23
Watch
11/03/23
Learn More
11/03/23
Watch
11/04/23
Learn More
11/04/23
Watch
11/05/23
Learn More
11/05/23
Watch
11/06/23
Read
11/06/23
Watch
11/06/23
Learn More
11/07/23
Watch
11/07/23
Read
11/07/23
Learn More
11/07/23
Read
11/08/23
Learn More
11/08/23
Watch
11/09/23
Watch
11/09/23
Watch
11/09/23
Learn More
11/10/23
Watch
11/10/23
Watch
11/10/23
Learn More
11/11/23
Watch
11/11/23
Watch
11/11/23
Learn More
11/12/23
Watch
11/12/23
Learn More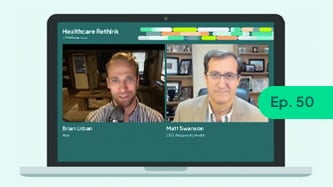
11/13/23
Watch
11/14/23
Watch
11/14/23
Watch
11/14/23
Read
11/14/23
Watch
11/14/23
Read
11/14/23
Watch
11/15/23
Watch
11/15/23
Read
11/15/23
Watch
11/16/23
Watch
11/21/23
Read
11/25/23
Read
11/30/23
Read
11/30/23
Read
12/10/23
Read
12/22/23
Watch
12/29/23
Watch
01/03/24
Watch
01/08/24
Watch
01/10/24
Watch
01/11/24
Read
01/11/24
Read
01/12/24
Watch
01/13/24
Watch
01/17/24
Watch
01/19/24
Watch
01/22/24
Watch
01/23/24
Read
01/23/24
Watch
01/25/24
Read
01/29/24
Read
01/31/24
Watch
02/02/24
Watch
02/03/24
Watch
02/06/24
Watch
02/07/24
Read
02/09/24
Read
02/09/24
Watch
02/09/24
Read
02/10/24
Read
02/20/24
Watch
02/23/24
Watch
02/23/24
Watch
02/23/24
Watch
02/26/24
Watch
02/26/24
Read
02/27/24
Watch
02/27/24
Read
02/29/24
Read
03/01/24
Watch
03/01/24
Watch
03/04/24
Read
03/04/24
Watch
03/05/24
Watch
03/05/24
Read
03/05/24
Read
03/07/24
Watch
03/08/24
Watch
03/11/24
Read
03/11/24
Read
03/14/24
Read
03/15/24
Watch
03/18/24
Watch
03/18/24
Read
03/18/24
Read
03/20/24
Read
03/22/24
Read
03/22/24
Watch
03/25/24
Watch
03/25/24
Read
03/26/24
Read
03/26/24
Watch
03/27/24
Read
03/28/24
Read
03/28/24
Watch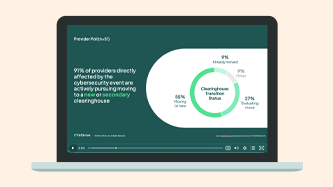
03/29/24
Watch
03/29/24
Watch
04/01/24
Watch
04/02/24
Learn More
04/05/24
Watch
04/05/24
Watch
04/08/24
Watch
04/12/24
Read
04/12/24
Read
04/12/24
Read
04/12/24
Watch
04/13/24
Read
04/15/24
Learn More
04/15/24
Watch
04/18/24
Read
04/19/24
Watch
04/22/24
Watch

